Does TMS Therapy work? (Data & Testimonials)
Clinically Reviewed by:
Large clinical studies consistently find that a significant portion of patients using Transcranial Magnetic Stimulation (TMS) experience meaningful symptom improvement, and some reach full remission.
Approximate Number of Studies
- 1,000+ peer-reviewed papers on TMS for depression alone.
- Hundreds of randomized controlled trials (RCTs).
- Thousands of studies have included anxiety, OCD, PTSD, stroke recovery, pain, and other neurological uses.
What the research is less clear about is why TMS therapy works well for some but not others. Depression and other mental health conditions involve complex brain circuits, genetics, and unique life factors. So, no one treatment works the same for everyone.
How successful is TMS therapy?
Across multiple clinical trials and real-world treatment studies most findings cluster around:
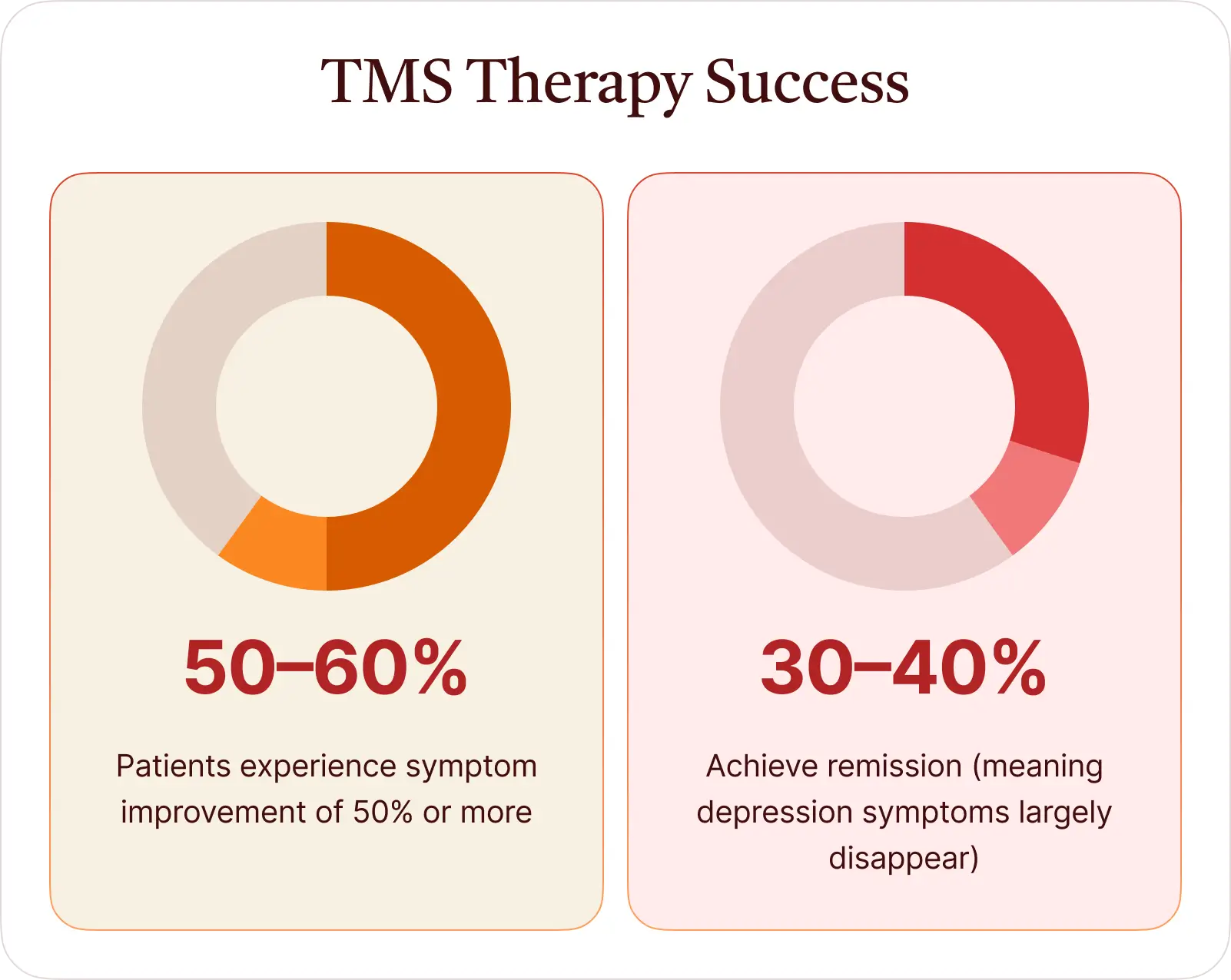
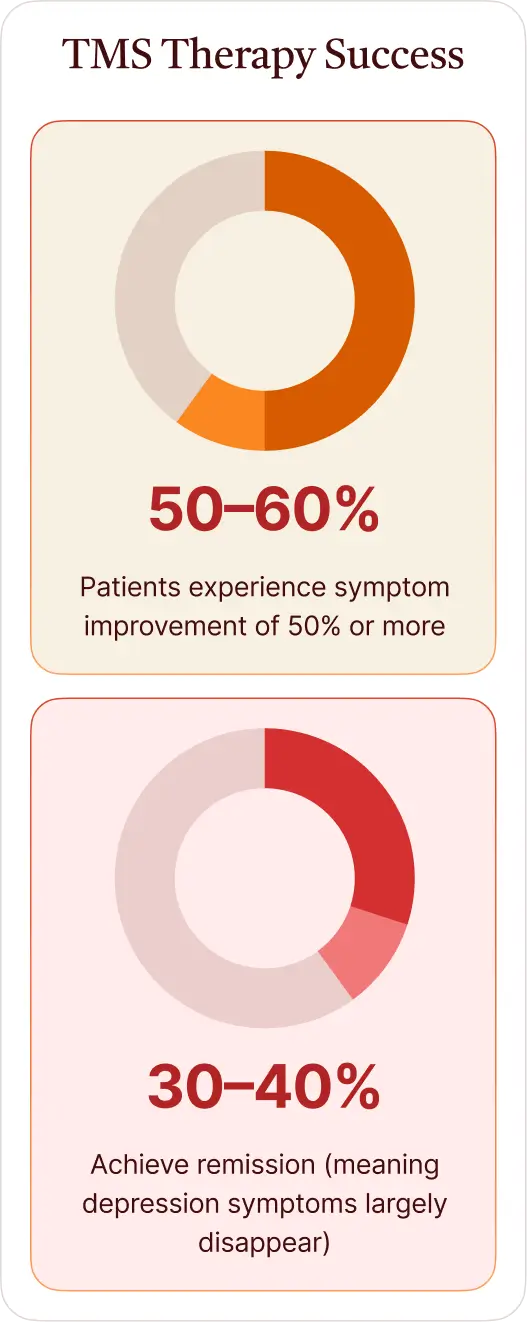
- 50–60% of patients experience symptom improvement of 50% or more.
- 30–40% achieve remission (meaning depression symptoms largely disappear).
Both outcomes represent meaningful improvement in people who previously struggled to respond to other treatments.
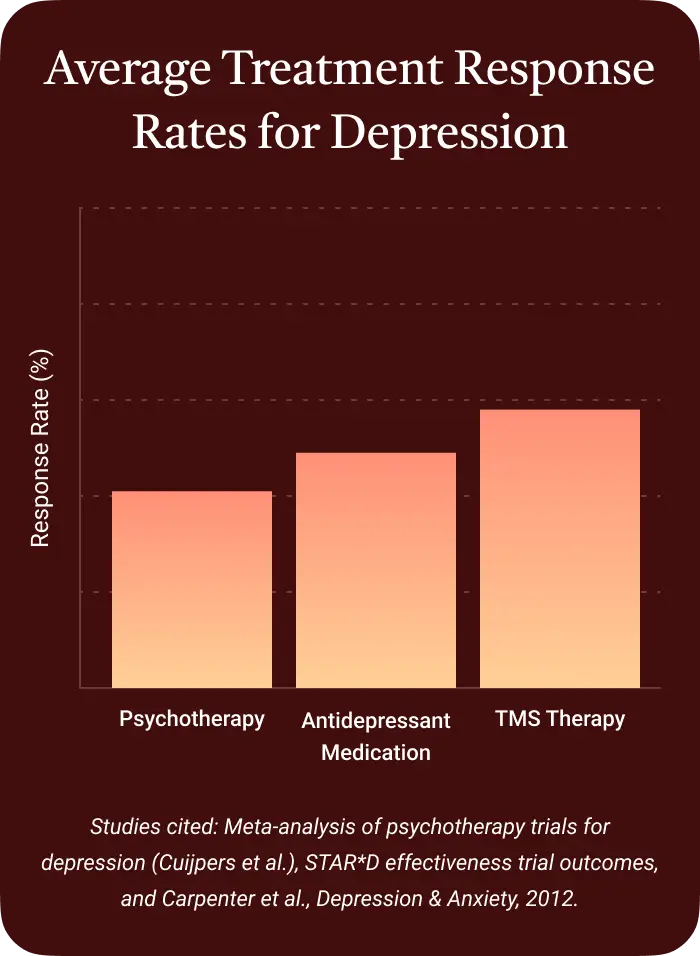
How effective is TMS therapy for depression?
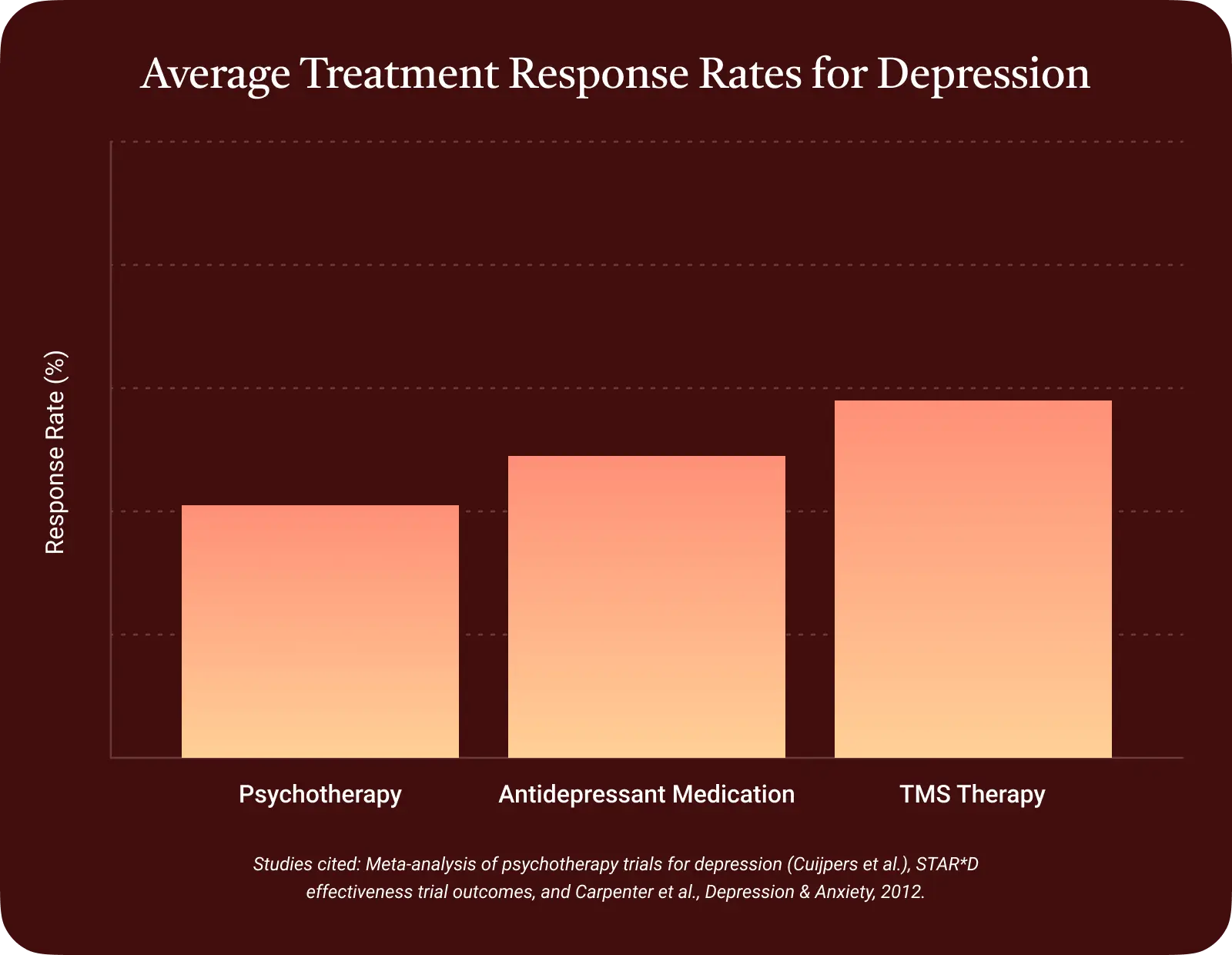
TMS therapy for depression is well supported by research and clinical evidence. In a 2013 meta-analysis of 29 studies, TMS produced 3-4 times greater remission rates than control patients, who were put into a TMS machine but not actually given the brain stimulation. ⓘ
While TMS can be effective when medication and psychotherapy (talk therapy) haven’t helped, over a dozen studies show that TMS used alongside antidepressants and talk therapy produce better outcomes than a singular treatment alone. ⓘ
- Antidepressant medications work completely differently on the brain, so the effects can complement each other.
- Talk therapy helps patients better use the improved brain plasticity created by TMS, reinforcing new emotional and cognitive patterns.
How effective is TMS therapy for anxiety?
TMS looks promising for anxiety, though there is much less data and the results aren’t as clear as for depression. A 2025 meta-analysis concluded that TMS combined with medication was more effective than the medication alone with no serious side effects or adverse events. ⓘ
Several studies suggest that patients with anxiety respond better to TMS if the anxiety occurs alongside depression, rather than an anxiety disorder alone. ⓘ
How effective is TMS therapy for PTSD?
TMS treatment shows promising results for PTSD, though there is less research than there is for depression. In a meta-analysis of 17 clinical studies, patients receiving TMS experienced significantly greater reductions in PTSD symptoms compared to control patients who received sham stimulation (a placebo version of the treatment that does not actually stimulate the brain).ⓘ
Researchers concluded that TMS may be an effective treatment for PTSD, but more studies are needed to determine which treatment protocols work best and which patients are most likely to benefit.
How effective is TMS therapy for bipolar disorder?
Several studies have found that TMS can produce meaningful improvements in bipolar depression, similar to results seen in major depressive disorder.
A systematic review analyzing 49 studies (1,593 patients) found that TMS showed meaningful improvements in bipolar depression symptoms, with response and remission rates similar to those seen in unipolar depression which, again, has been heavily studied.ⓘ
TMS is not used during manic or hypomanic episodes, because stimulation could worsen mania in some patients.
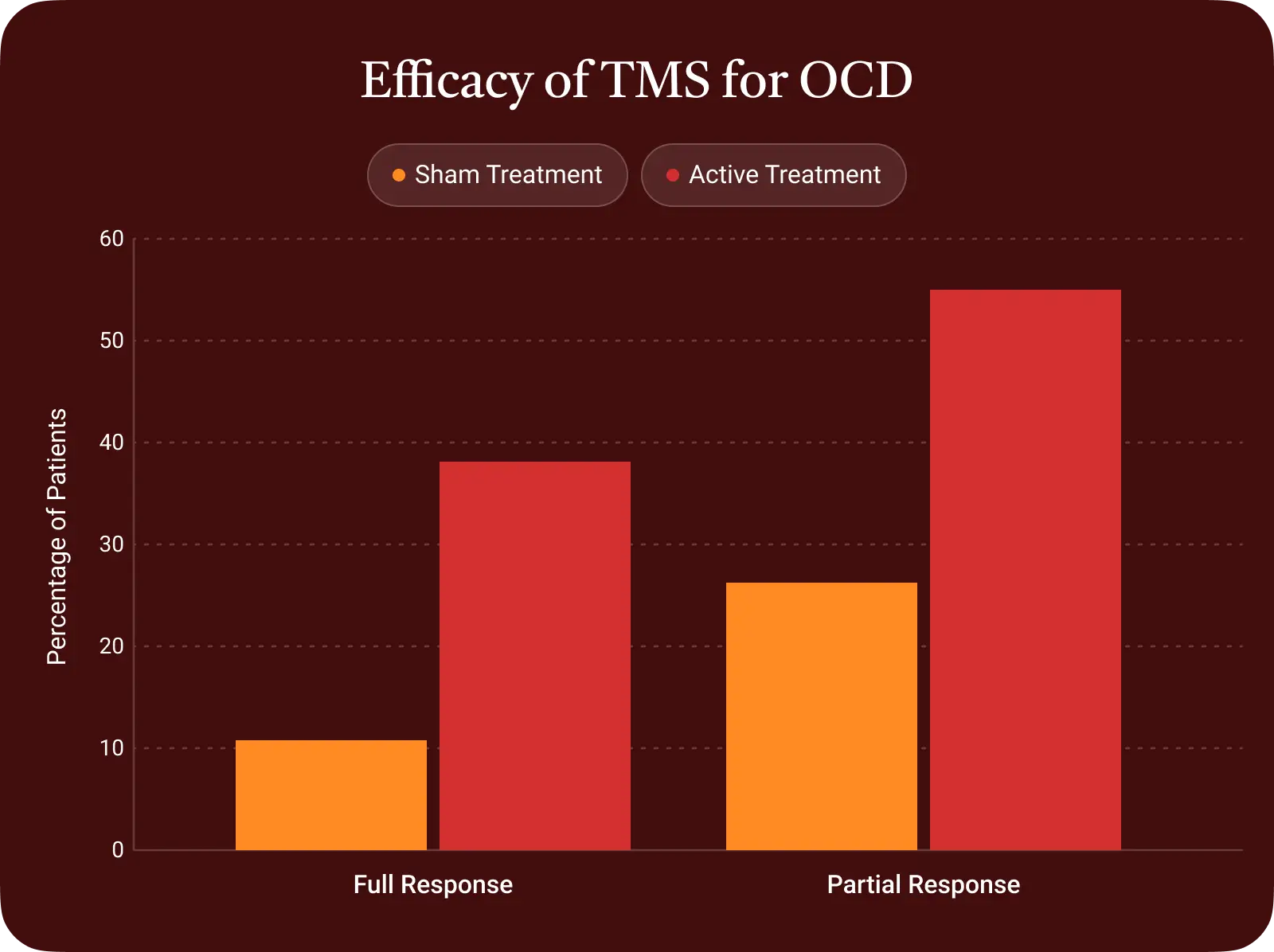
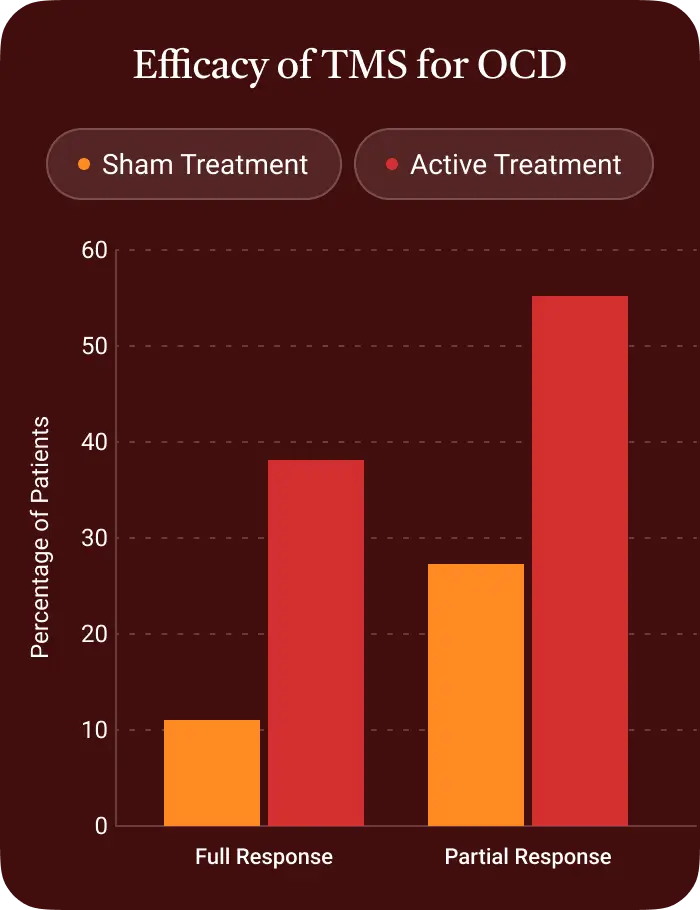
How effective is TMS therapy for OCD?
TMS is effective enough for OCD that there is an FDA-cleared protocol.ⓘ The evidence base is stronger than it is for anxiety or PTSD.
In a 2023 meta-analysis of 25 randomized controlled trials, patients receiving TMS were about 3 times more likely to experience meaningful improvement in OCD symptoms compared to control patients who did not receive real brain stimulation.ⓘ
The same analysis also found that OCD patients with depression improved more, which may explain why some patients respond better than others.
Frequently Asked Questions (FAQ)
What makes TMS more likely to be successful?
Research suggests TMS is more likely to work when:
- The current depressive episode is shorter
- Fewer antidepressant medications have failed
- Patients show early symptom improvement during the first couple of weeks of treatment
Several studies suggest that patients with both depression and severe anxiety are less likely to achieve remission in depression-focused TMS protocols. Though this is not absolute and many patients with anxiety or complex symptoms still respond very well.
Other factors that influence outcomes:
- Completing the full treatment course
- Accurate brain targeting
- Supportive therapy (Participating in therapy during TMS treatment, managing stress, and getting good sleep also influence how strongly symptoms improve)
How soon do most people notice improvement?
Most patients notice some improvement between weeks 2 and 4 of treatment.
Weeks 1–2: little change for many patients
Weeks 2–4: early improvements such as better sleep or energy
Weeks 4–6: clearer mood improvement and reduced symptoms
Some people respond earlier, while others do not notice major changes until the end of the treatment course.
What does it feel like when TMS starts working?
TMS changes are often subtle at first. Many patients describe noticing small improvements in daily functioning before their mood fully improves.
Common early signs include:
- Sleeping better or falling asleep easier
- Getting out of bed with less effort
- Less constant negative thinking or rumination
- Feeling slightly more motivated to do normal activities
- Reduced irritability or emotional overwhelm
For many people, improvement builds gradually over several weeks as the brain’s mood-regulation circuits become more active.
How long do TMS results last?
TMS results can last for months, especially when patients complete a full TMS therapy treatment course and respond well early on. However, relapse happens for a portion of patients, which is where maintenance sessions can help.
- A 2023 meta-analysis found that depression scores remain improved for at least 3 months after TMS, though outcomes were better when maintenance TMS was used. ⓘ
Research suggests the first year is the most fragile, so follow-up care matters.
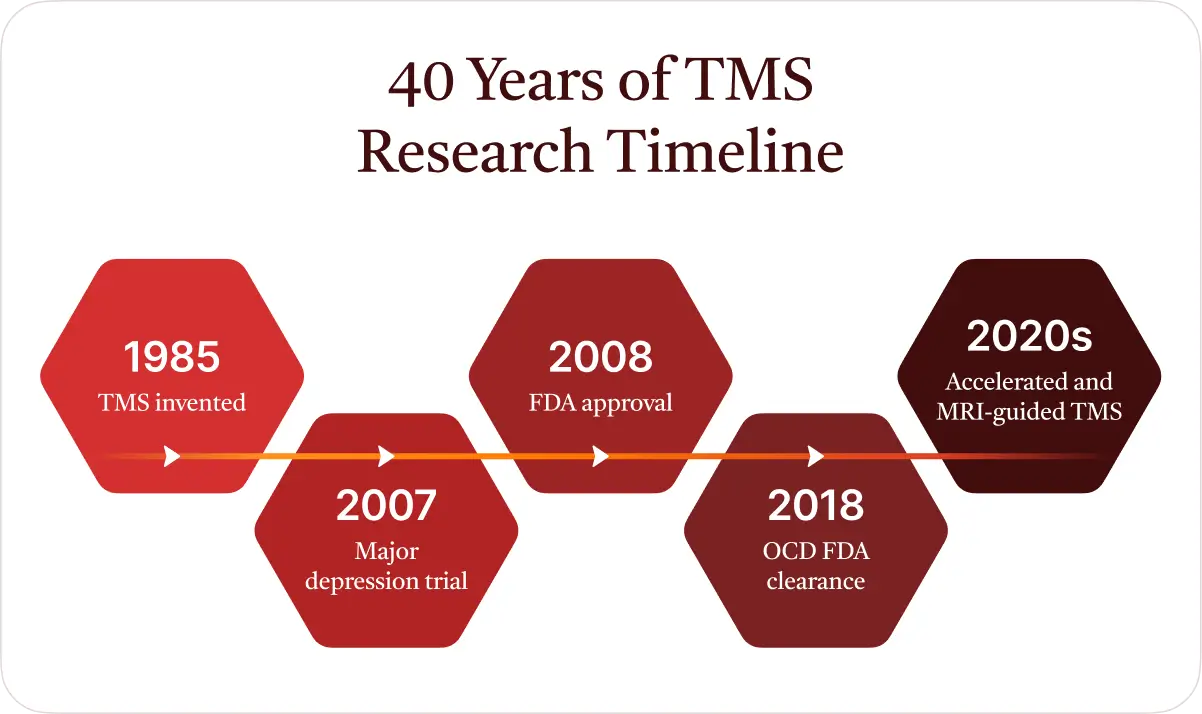
How long has TMS therapy been around?
TMS was first developed in 1985 by researchers at the University of Sheffield in the United Kingdom. It was later approved by the U.S. FDA for depression in 2008.
Since then, the technology and treatment protocols have improved significantly, and it is now considered an innovative evidence-based treatment option.
What are the major studies on TMS?
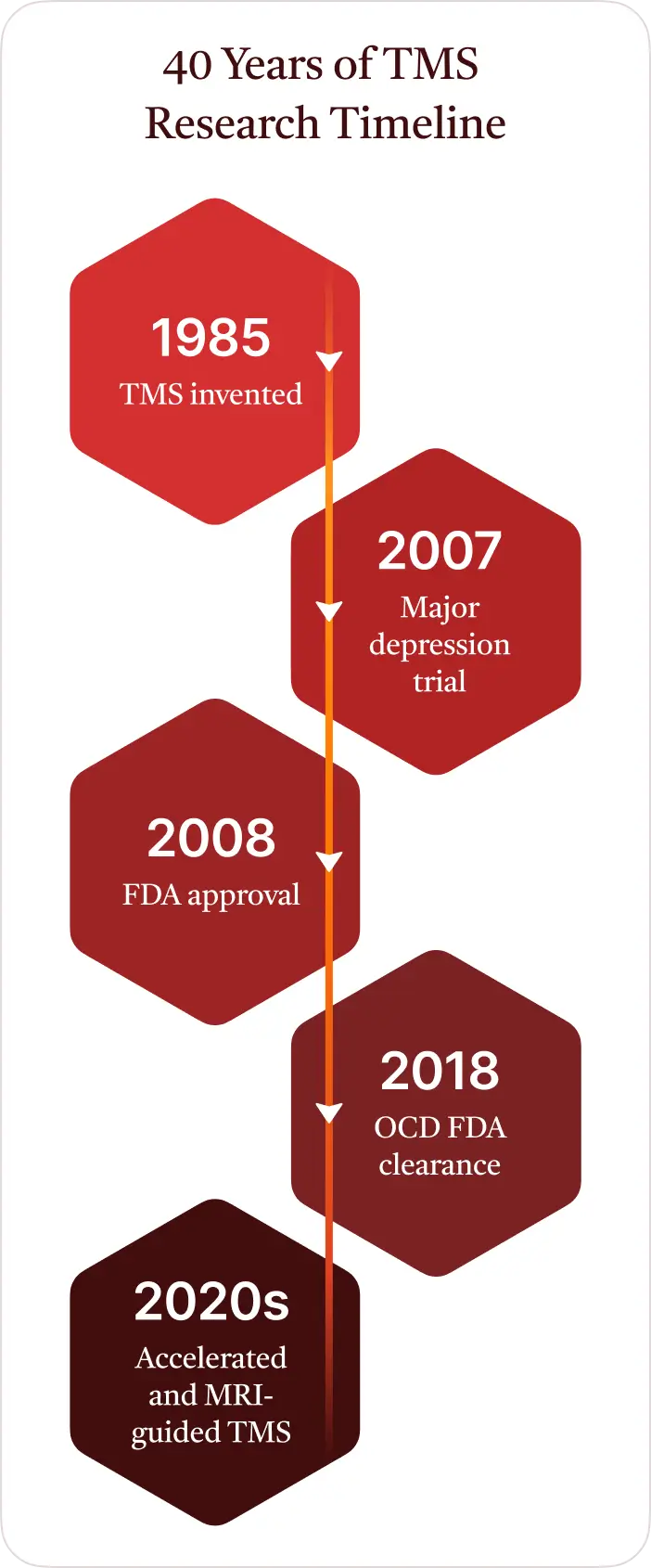
Research on TMS has been ongoing for more than 40 years. Scientists and clinicians have conducted thousands of studies evaluating how TMS works and which patients benefit most. Over time, this research has expanded beyond depression while also testing different stimulation targets, treatment schedules, and newer protocols such as accelerated and MRI-guided TMS.
The list below highlights the 10 most cited studies that helped establish TMS as a legitimate medical treatment and continue to shape how it is used today.
- 1985 The Lancet: First demonstration of non-invasive magnetic stimulation of the human brain, introducing the technology that later became Transcranial Magnetic Stimulation (TMS). https://doi.org/10.1016/S0140-6736(85)92413-4
- 2007 Biological Psychiatry: A randomized controlled trial that showed significant symptom improvement and led to FDA clearance of TMS for depression. https://doi.org/10.1016/j.biopsych.2007.01.018
- 2012 Depression and Anxiety: A real-world study across 42 clinics found 58% response and 37% remission rates in patients with major depressive disorder treated with TMS. https://doi.org/10.1002/da.21969
- 2019 American Journal of Psychiatry: A prospective multicenter randomized, double-blind trial found that deep TMS significantly improved OCD symptoms compared to sham treatment, helping establish the evidence base that led to FDA clearance for OCD. https://doi.org/10.1176/appi.ajp.2019.18101180
- 2020 Clinical Neurophysiology: Evidence-based international guidelines reviewing hundreds of trials concluded that TMS is an effective treatment for treatment-resistant depression with strong clinical support. https://doi.org/10.1016/j.clinph.2019.11.002
- 2020 The Lancet EClinicalMedicine: Large analysis of TMS treatment outcomes confirmed it as an evidence-based therapy for major depressive disorder and examined predictors of patient response. https://www.thelancet.com/journals/eclinm/article/PIIS2589-5370(20)30093-6/fulltext
- 2021 UCLA Semel Institute: Real-world clinical outcomes showed more than half of patients experienced meaningful improvement with TMS even after failing antidepressant medications. https://www.uclahealth.org/news/release/study-finds-possible-early-predictor-successful-transcranial
- 2024 Randomized Controlled Trial (Dalhuisen et al.): Compared rTMS to switching antidepressants and found rTMS produced better outcomes for treatment-resistant depression. https://med.uth.edu/psychiatry/2025/03/17/rtms-vs-antidepressants-a-new-path-for-treatment-resistant-depression/
- 2025 JAMA Network: Found maintenance TMS prevented relapse at rates comparable to lithium while producing fewer adverse effects. https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2835319
- 2025 Brain Stimulation: Accelerated dual-target stimulation protocols showed improved response rates for major depressive disorder using advanced brain targeting. https://www.sciencedirect.com/science/article/pii/S2666379125004756
Is TMS therapy legit?
Yes. TMS is a well-studied medical treatment that has been cleared by the FDA for several conditions, including:
- Major depressive disorder
- Obsessive-compulsive disorder (OCD)
- Smoking cessation
TMS is also commonly used off-label for other mental health conditions when standard treatments have not worked because research shows potential benefit and the treatment is considered safe. Research and clinical practice suggest it may help with:
- Anxiety disorders (especially when anxiety occurs alongside depression)
- PTSD and trauma-related conditions (where studies show meaningful reductions in symptoms)
- Bipolar depression (though it is usually avoided during manic episodes)
There are now thousands of research studies and hundreds of clinical trials evaluating TMS.
How can I get TMS therapy near me?
Not all treatment centers offer TMS. When looking for a provider, consider providers that offer:
- FDA-cleared TMS devices
- Experienced psychiatrists who specialize in neuromodulation treatments
- Insurance verification for TMS therapy
- Additional therapies in case TMS is not the best fit
If you’re in or near Indiana, Indiana Center for Recovery is often considered the best option in the Midwest for serious mental health issues. ICFR offers TMS therapy along with other advanced mental health treatment options to find the approach that works best for your specific symptoms, including:
- TMS Therapy
- Ketamine Therapy
- GeneSight genetic testing to guide medication choices
- Biofeedback therapy
- EMDR trauma therapy
Patients also have access to more dedicated evidence-based talk therapies and holistic therapies such as acupuncture, reiki and equine therapy.
Having multiple treatment options in one place means you don’t have to put all your hope into just one option like TMS. Even if TMS doesn’t work for you, there are plenty of other breakthrough treatment options that can.
Call today to learn more without commitment and 100% confidential.
Indiana Center for Recovery Locations





 100% Confidential
100% Confidential
