
TMS vs. Ketamine Therapy – Which Treatment Is Best For You?
Clinically Reviewed by:
When mental health symptoms don’t improve after standard medications and therapies, it’s time to look for additional options. The two most common evidence-based advanced options are:
These treatments work in very different ways and can even be used together. The right option depends on how severe the symptoms are, how quickly relief is needed, what other conditions are at play, and what treatments have already been tried.
TMS vs. Ketamine Overview
How It Works
A machine uses targeted magnetic pulses to stimulate areas of the brain linked to mood regulation to restore normal activity in the prefrontal cortex.
The medication ketamine affects the glutamate system to help the brain create new neural connections.
What It’s Like
Patient sits in a chair. The device is placed on the head. Sessions last about 18–30 minutes.
ICFR administers a nasal spray (Spravato). Treatment is monitored in-office. Sessions last 40–60 minutes, followed by observation while the medication wears off.
Results Timeline
Improvement usually happens gradually over several weeks of treatment.
Can improve symptoms quickly, sometimes even after one session, though multiple treatments are often needed.
Side Effects
Mild scalp discomfort, headache, or tingling during treatment. Side effects are usually temporary and resolve shortly after the session.
Temporary dissociation, dizziness, nausea, or increased blood pressure during treatment. Effects typically fade within a few hours.
Recommended For
- Depression that hasn’t improved with antidepressants
- Depression with anxiety symptoms
- OCD (FDA-cleared)
- Depression that hasn’t improved with antidepressants
- Depression with anxiety symptoms
- Suicidal ideation or severe symptoms needing rapid relief
Key Benefit
No medication
Fast symptom relief
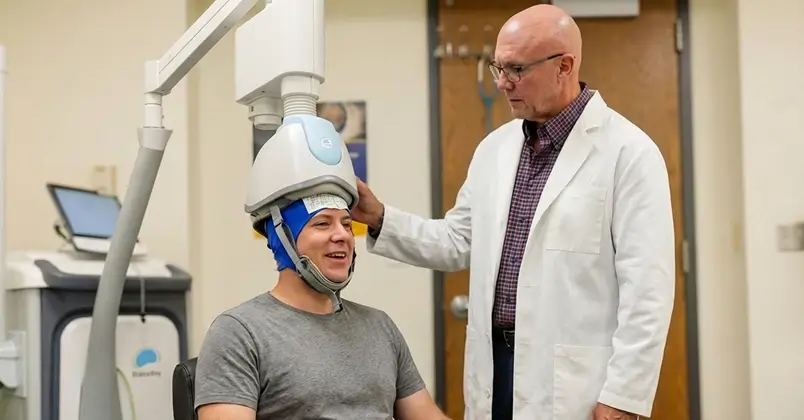 TMS Therapy
TMS TherapyHow It Works
A machine uses targeted magnetic pulses to stimulate areas of the brain linked to mood regulation to restore normal activity in the prefrontal cortex.
What It’s Like
Patient sits in a chair. The device is placed on the head. Sessions last about 18–30 minutes.
Results Timeline
Improvement usually happens gradually over several weeks of treatment.
Side Effects
Mild scalp discomfort, headache, or tingling during treatment. Side effects are usually temporary and resolve shortly after the session.
Recommended For
- Depression that hasn’t improved with antidepressants
- Depression with anxiety symptoms
- OCD (FDA-cleared)
Key Benefit
No medication
 Ketamine Therapy
Ketamine TherapyHow It Works
The medication ketamine affects the glutamate system to help the brain create new neural connections.
What It’s Like
ICFR administers a nasal spray (Spravato). Treatment is monitored in-office. Sessions last 40–60 minutes, followed by observation while the medication wears off.
Results Timeline
Can improve symptoms quickly, sometimes even after one session, though multiple treatments are often needed.
Side Effects
Temporary dissociation, dizziness, nausea, or increased blood pressure during treatment. Effects typically fade within a few hours.
Recommended For
- Depression that hasn’t improved with antidepressants
- Depression with anxiety symptoms
- Suicidal ideation or severe symptoms needing rapid relief
Key Benefit
Fast symptom relief
TMS vs. Ketamine for Depression
Both TMS therapy and ketamine therapy can be great options when depression does not improve with two or more standard antidepressant medications (known as treatment-resistant depression).
TMS Is Often Recommended First
TMS is often recommended before Ketamine because it has been studied extensively with a long track record of helping people with treatment-resistant depression. It also does not involve medication, which means fewer systemic side effects. ⓘ
TMS advantages include:
- More predictable results
- Generally mild, temporary side effects
- More likely to be covered by insurance
- Long-lasting symptom improvement for many patients
- Strong research support for depression treatment
However, TMS usually works gradually. Most patients notice improvement after several weeks of treatment as the brain’s mood-regulating circuits become more active. ⓘ
When Ketamine Therapy May Be Recommended First
Ketamine therapy may be recommended before TMS if depression symptoms are severe or when faster relief is needed. Unlike traditional antidepressants that work on serotonin, ketamine acts on the brain’s glutamate system, which can yield much more immediate results for some patients.
Ketamine advantages include:
- Much faster symptom relief for many patients, sometimes within hours or days
- Can reduce suicidal thoughts quickly in some patients
- Can help some patients who did not respond to TMS
However, the effects of ketamine may not last as long without follow-up treatments. Many patients require maintenance sessions to keep symptoms under control. ⓘ
TMS vs. Ketamine for Anxiety
Both TMS therapy and ketamine therapy may be considered when anxiety symptoms do not improve with standard treatments such as medication and therapy. This can include conditions like generalized anxiety disorder, panic disorder, and especially anxiety that occurs alongside depression.
TMS Is Often Recommended First
TMS is often recommended before ketamine for anxiety-related symptoms because it has a longer clinical track record and does not involve medication. Stimulating areas of the brain involved in emotional regulation can help both depression and anxiety symptoms. ⓘ
TMS therapy is also more likely to be covered by insurance and tends to produce fewer side effects and more predictable results.
TMS is most commonly used when anxiety occurs alongside depression, since the treatment targets brain regions involved in mood regulation that influence both conditions.
Because the treatment gradually improves brain activity over several weeks, patients often notice reduced rumination, fewer panic symptoms, and better emotional regulation over time.
When Ketamine Therapy Is Recommended
Ketamine therapy may be recommended before or alongside TMS when anxiety symptoms are severe and require rapid relief, or when significant depression symptoms are also present, including suicidal ideation. ⓘ
Because ketamine affects the brain’s glutamate system, some patients experience a rapid reduction in anxiety intensity and intrusive negative thinking.
Ketamine may also be considered when panic symptoms or severe emotional distress require faster stabilization.
However, ketamine research for anxiety disorders is still developing, and results may be temporary without maintenance treatments.
TMS vs. Ketamine for OCD
Both TMS therapy and ketamine therapy may be considered when obsessive-compulsive disorder (OCD) does not improve with standard treatments such as selective serotonin reuptake inhibitors (SSRIs) and exposure and response prevention (ERP) therapy, which are the most common behavioral treatments for OCD.
TMS Is Often Recommended First
TMS is often recommended before ketamine for OCD because it has an FDA-cleared treatment protocol specifically for OCD. The treatment targets brain circuits involved in compulsive behaviors and intrusive thoughts. ⓘ
By stimulating these areas of the brain, TMS can help reduce the intensity of obsessions and make it easier for patients to resist compulsive behaviors.
TMS therapy is also more likely to be covered by insurance and tends to produce predictable, gradual improvement with relatively mild side effects.
TMS protocols for OCD require specialized targeting and longer sessions compared to depression protocols.
When Ketamine Therapy Is Recommended
TMS currently has stronger research support for treating OCD and is typically considered first.
Ketamine therapy may be considered when OCD symptoms remain severe and disabling after multiple medications and therapies have not worked, or when faster symptom relief is needed. Because ketamine affects the brain’s glutamate system, some patients experience a rapid reduction in obsessive thinking in the short term. ⓘ
Ketamine research for OCD is still developing and results may be temporary.
TMS vs. Ketamine for PTSD
Neither TMS nor ketamine is currently FDA-cleared specifically for post-traumatic stress disorder PTSD, though both are used clinically when first-line treatments like trauma-focused therapies and antidepressant medications have not helped.
These treatments are often explored when symptoms like intrusive memories, emotional numbness, hypervigilance, or severe anxiety continue despite therapy and medication.
TMS Is Often Recommended First
TMS is sometimes recommended before ketamine for PTSD because it has a longer safety track record and does not involve medication. The treatment stimulates brain regions involved in emotional regulation and stress response, which can help reduce symptoms such as hyperarousal and negative mood.
TMS therapy is also more likely to be covered by insurance and tends to produce predictable, gradual improvement with relatively mild side effects.
Some patients experience improvements in sleep, mood regulation, and reduction of trauma-related anxiety as treatment progresses. ⓘ
When Ketamine Therapy Is Recommended
Ketamine therapy may be recommended before or alongside TMS when PTSD symptoms are severe or require faster stabilization, particularly when symptoms include suicidal thoughts or severe depression.
Because ketamine affects the brain’s glutamate system, some patients experience rapid improvements in mood and reductions in trauma-related distress.
Ketamine may also help reduce intrusive thoughts and emotional intensity related to traumatic memories in the short term.
However, research on ketamine for PTSD is still developing, and symptom improvement may require ongoing or maintenance treatments. ⓘ
TMS vs. Ketamine Patient Feedback
I was iffy about TMS but so far I’m feeling okay with the results. It’s nbd really. My insomnia is vaporized. I’m sleeping without heavy drugs to sedate me. I’m cooking again, eating normal food not scraping to get by with my depression laying around all day. I’m saving ketamine for a psych emergency.
TMS definitely did the trick. Is my depression gone? No, but TMS brought me from the depths of despair. I had given up and was going to let it win. Now, I am now actively working to better my situation and can function like a normal person, not some volatile jerk. My anxiety was out of control, and when I’m anxious I lose my temper easily. Now, I feel mostly calm. Do things still upset me? Yes, but I can react appropriately. I would do it again. I wish TMS had been an option for me when I was younger.
I did TMS last summer. At the time, I was suicidal nearly every day. After treatment my phq9 was 0. I felt amazing. Over two years later, I have not had any SI or self-harm. I’ve been off meds for a year now. I still have a low day sometimes. But “low” now means I can still get out of bed, do my everyday life stuff, and see potential joy in life. Nothing like it ever was before. I am motivated to keep living and excited for what the next day brings.
I was grateful for ketamine because it gave me the mental space to deal with the stuff happening in my life. By the time I went for treatments, I wasn’t functioning at all. It’s easy for people to say, “Hey, get some help!” but if you’re not able to function, you don’t have the energy to deal with the American mental health system. Ketamine helped with the depression and I finally got some sleep and didn’t wake up with an anxiety attack. The usual things upset me, but after ketamine, it was if my brain was able to put them in their proper perspective. I bounced back quicker from adverse events. I became more social and more active.
TMS did nothing for me. Ketamine has helped. After my first session without a doubt I could see a clear path to improve my rapid cycling depression. It’s an incredible tool to heal.
I personally didn’t have time to do extra treatments because my depression was so bad. I had ketamine and in three sessions my depression was cured. It was simple and extremely effective for my very, very severe depression.
Get TMS & Ketamine Therapies
When depression, anxiety, OCD, or PTSD do not improve with standard treatment, a different approach is needed.
At Indiana Center for Recovery, mental health treatment is not limited to a single method. Both TMS therapy and ketamine therapy are available, along with other advanced options designed to help when traditional treatments have not worked.
Advanced treatments available include:
- TMS Therapy
- Ketamine Therapy
- GeneSight Genetic Testing, which helps identify mental health medications that may work better with your specific genetics
- Biofeedback, which helps retrain the nervous system to regulate stress and emotional responses
- EMDR Therapy, a trauma-focused treatment that helps process distressing memories
Treatment can also include gold standard therapies like Cognitive Behavioral Therapy (CBT), Acceptance and Commitment Therapy (ACT), and Dialectical Behavior Therapy (DBT) – as well as holistic options like acupuncture, reiki, and equine therapy.
The wide range of evidence-based treatment options allows treatment to be tailored to you instead of pushing one standard program. For many, a breakthrough comes when the right combination of therapies is finally used.
Even if previous treatments have not worked, advanced options like TMS or ketamine can still help. Call in any time to talk through your situation without commitment.
Indiana Center for Recovery Locations





 100% Confidential
100% Confidential
